
Cashless claim settlement facilities have become so convenient for policyholders as they need not spend hefty amounts upfront for treatments. Even after two decades of health insurance in the country, policyholders are still filing for reimbursement claims for various reasons.
What’s on this page?
Broadly, There are Two Reasons Pushing Policyholders to File Reimbursement Claims in Our Country:
- There is a lack of network hospitals in the policyholders’ locations. If we look at the network hospital list, we find that around 80-90% of these hospitals are in Tier 1 cities, and only a few are in Tier 2 and Tier 3 cities. Even though the hospitals are making their way to Tier 2 and 3 cities, there is a lot more work to be done in these areas.
- Cashless claim insurance rejection/ denial by the insurance company. It could happen for various reasons, which are mentioned here.
However, it is important to learn the cashless claim settlement process so that one can be confident at the time of hospitalization. Let’s discuss the step-by-step process of cashless claim settlement in India.
Cashless Claim Settlement Step by Step Process
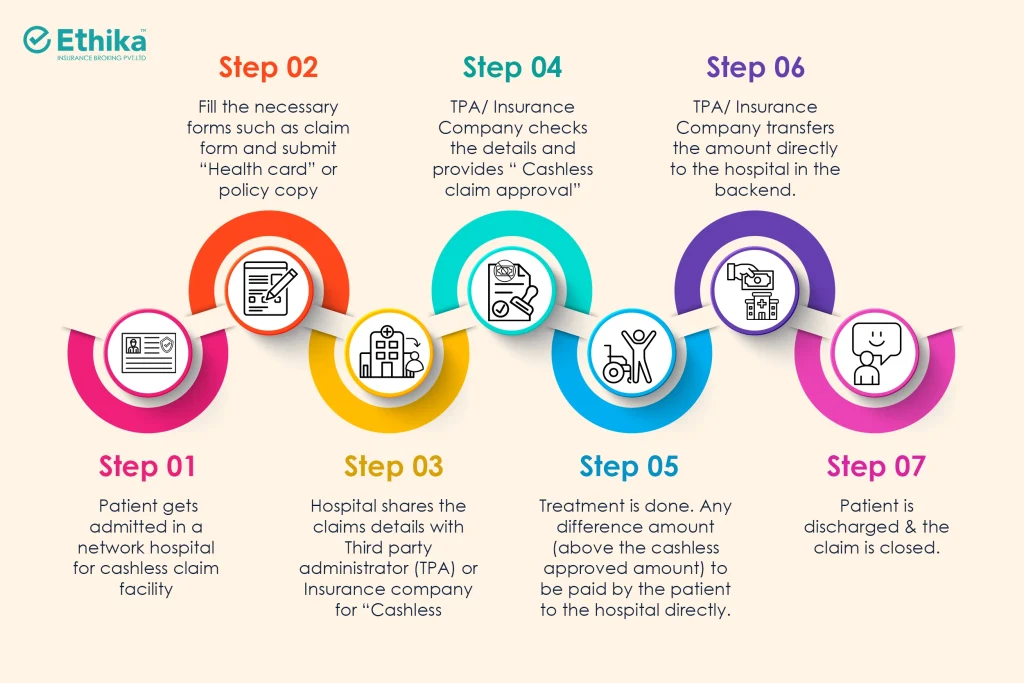
| Step 1: Patient gets admitted in a network hospital for cashless claim facility |
⬇
| Step 2: Fill the necessary forms such as claim form and submit “Health card” or policy copy |
⬇
| Step 3: Hospital shares the claims details with Third party administrator (TPA) or Insurance company for “Cashless Approval” |
⬇
| Step 4: TPA/ Insurance Company checks the details and provides “ Cashless claim approval” |
⬇
| Step 5: Treatment is done. Any difference amount (above the cashless approved amount) to be paid by the patient to the hospital directly. |
⬇
| Step 6: TPA/ Insurance Company transfers the amount directly to the hospital in the backend. |
⬇
| Step 7: Patient is discharged & the claim is closed. |
However, the current cashless claim settlement process in India has some drawbacks. The first and most important is that each insurance company has tied up with multiple hospitals, limiting the number of hospitals on their network based on their size. India’s insurance regulatory and development authority and the government have proposed a 100% cashless claim settlement facility for all health insurance policyholders to overcome this issue. IRDAI plans to onboard all the hospitals to provide a cashless claim settlement facility, which could be utilized by all the policyholders, irrespective of their insurer.
FAQs
Can I avail of reimbursement in a network hospital?
Yes. You may receive reimbursement in a network hospital only if your cashless claim was not approved on time. If there are chances of cashless approval and you still choose to receive reimbursement, insurance companies might include a copayment in the claim.
What is the usual time period for a cashless approval?
A cashless approval could be obtained in as little as 30 minutes and as long as 24 hours. It all depends on the hospital’s processing time and the TPA/ Insurance company’s. The insurance company might require different documents before granting cashless claim approval. If all these documents are provided on time, then the cashless facility will be approved immediately.
Can I get a cashless claim if I don't have a health card?
Yes. You can use the cashless claim settlement facility even though you do not have a health card. Your health insurance policy serves as proof of contract.
Which one is better- Cashless or Reimbursement?
On any day, cashless claim settlement is superior to reimbursement claim settlement. In cashless claim settlement, the entire claim filing process is taken care of by the hospital, whereas in reimbursement claims, policyholders need to file the claim, follow up, and settle it.
What to do if the cashless claim approval is late?
In case of delay in receiving cashless claim approval, you should coordinate with the hospital, TPA, and insurance company to speed up the approval process.